Research Overview
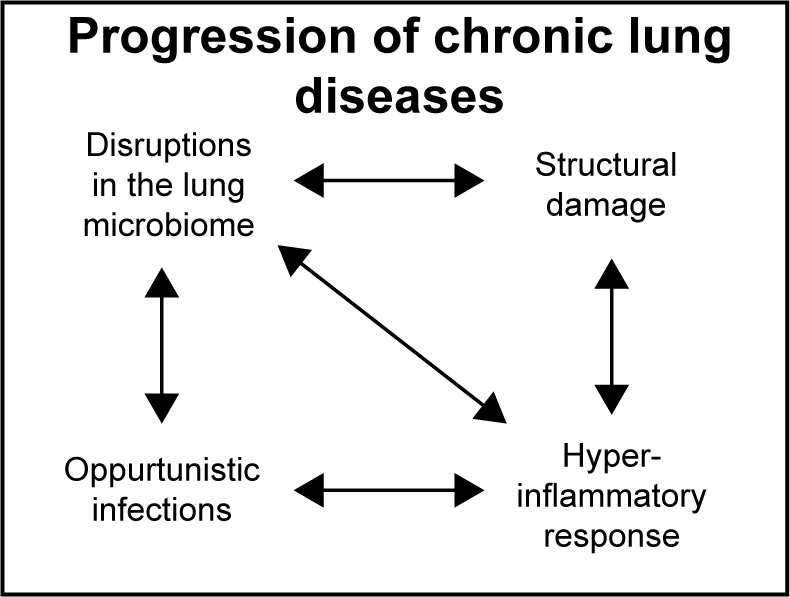
Respiratory diseases remain a leading cause of global morbidity and mortality despite many advances in medicine. The pathology underlying many chronic lung diseases is incredibly complex, and disease progression occurs through an interplay of various factors, including the composition of lung microbiome, the architecture of the airways, and immune response to opportunistic microbes. Inhaled drug delivery is well-suited for the treatment of respiratory diseases as it eliminates the need for plasma-to-lesion or infection-site distribution. However, the complex pathology underlying many chronic lung diseases presents numerous challenges for successful drug delivery. The Brunaugh Lab is focused on the elucidation of the underlying mechanisms for respiratory disease progression to determine appropriate therapeutic targets and develop novel formulation and inhaled drug delivery approaches to improve patient outcomes. We are interested in the development and optimization of both nasal and orally inhaled drug products.
Research Area #1: Identify appropriate targets for inhaled drug delivery
Our airways are constantly exposed to opportunistic pathogens and environmental toxins. As such, a robust defense system is in place which consists of both physical barriers as well as a complex and interconnected innate immune response. However, an overexuberant inflammatory response can result in development of acute lung injury or progressive pulmonary function decline in chronic lung diseases. Understanding these changes relative to normal function can enable identification of new therapeutic targets, though reaching those targets requires that we overcome the same physical defense systems which help block pathogens. In this area of the Brunaugh Lab's research, we are interested in investigating host immune responses to environmental toxins and pathogens (bacterial, viral, fungal) as well as understanding the role of the airway microbiome in dysfunctional or hyperinflammatory immune responses. Through this, we seek to identify suitable compounds for drug repurposing, screen synergistic combinations of drugs, and guide formulation design by minimizing excipients which may induce an unexpected inflammatory response in the diseased lung.
Research Area #2: Develop improved in vitro and in vivo models for inhaled drug delivery
Within this area of the lab's research, we seek to understand why inhaled therapies sometimes fail, particularly those that fall ou tside the historical inhaled therapeutic space of small, potent molecules for asthma / COPD. To more accurately predict the fate of the drug after lung deposition, we are working to develop improved in vitro, in vivo and in silico models to investigate drug - mucus interations, drug-biofilm interacitons, phagocyte clearance of drug, and absorption through epithelial barriers in variety of pulmonary disease states. The results of these studies guide our particle engineering and formulation design efforts to improve inhaled drug product performance and de-risk movement from preclinical to clinical stages of development.
Research Area #3: Optimize inhaled drug product design
The design of inhaled drug products that are safe and therapeutically effective is extremely challenging due to the limited number of FDA-approved excipients for inhalation and the complex interactions that exist between formulation and device that can alter product performance unexpectedly. Guided by studies performed as part of research area 1 and 2, we use a variety of particle engineering techniques (spray drying, spray freeze drying, anti-solvent precipitation, milling) to develop "next-generation" inhaled formulations that incorporate repurposed small-molecules, labile biologics, and synergistic drug combinations and that exhibit appropriate safety profiles, stability in challenging environments, fine-tuned drug release to achieve desired PK/PD profiles, and are robust to patient factors like reduced pulmonary function